There are plenty of small things that happen to us that we never really give much thought to. For example, have you ever gotten those cracks in the corner of the mouth? They tend to be a little stiff and blistery. Did you know there’s an actual name for those and that those cracks are treatable? Those cracks are called angular cheilitis.
- Itchy lips, cracked, chapped and dry lips are all few conditions that cause extreme pain and irritation to the sufferer unnecessarily and are usually easily curable. Peeling lips is another similar problem, where the skin of the lips begins to peel out due to dryness and lack of moisturization which later causes a burning sensation.
- It is usually seen in inflammatory skin conditions particularly when the skin is severely cracked or peeling. Infections may also a problem. Shingles (herpes zoster) is a reactivation of the chickenpox virus which causes neuralgia. It is mainly seen on the upper body and can involve the hands as well as the fingers.
Dec 25, 2018. Jan 16, 2018.
In this article, we will take a look at angular cheilitis causes, angular cheilitis symptoms, and angular cheilitis treatment. We even have home remedies to help get rid of those pesky cracks. Hopefully, by the end, you’ll be able to notice those cracks earlier and clean them up before anyone else notices.
What Causes Cracks in Corner of Mouth
So, we now know that the cracks in the corner of the mouth are called angular cheilitis. But what causes angular cheilitis? What are the things that lead to those cracks in the corners of your mouth?
There are a few causes of angular cheilitis.
1. Saliva
It may seem odd, but yes, your own saliva can cause the cracks in the corner of the mouth. The moisture from saliva gets trapped in those corners and becomes fertile ground for fungus and bacteria. This can be a common issue for people with braces or dentures.
2. Fungus
It may seem gross and brings to mind images of small mushrooms growing out of your face but it’s true, angular cheilitis is usually a result of a fungal infection. In particular, it’s caused by a yeast called Candida. Parents might recognize Candida as the fungal infection that causes diaper rash in babies.
3. Bacterial Infection
As noted above, trapped saliva can attract bacteria that can cause the cracks and slight blistering at the corner of your mouth.
4. Dehydration

The cracking at the corners of your mouth might just be due to dehydration. If you don’t get enough fluid into your system, your skin can start to dry out a little, including the corners of your mouth.
Now that you know what causes the cracks in the corner of the mouth, it’s time to look at what you can do to try to treat them.
How to Treat Cracks in Corner of Mouth
While angular cheilitis can be kind of gross to have or to look at, luckily, there are some medical options for you to use to get those pesky cracks to go away.
1. Anti-Fungal Cream
As we noticed in the previous section, the most prevalent cause of angular cheilitis is a fungal infection. Luckily, there are some over-the-counter anti-fungal creams that can help clear up the fungal infection. If the infection is particularly stubborn, there are prescription creams that can help move the fungus out of the corners of the mouth.
2. Zinc Oxide Paste
Zinc oxide paste can help repair the damage of the cracked corners of your mouth. It works especially well if the damage is a result of dehydration.
3. Good Oral Hygiene
A lot of the bacteria that can cause angular cheilitis originates in the mouth. To combat this, just keep up good oral hygiene. If you brush and floss properly and use mouthwash, it will eliminate a lot of the bacteria that will cause the cracks in the corners of the mouth.
Also, make sure your dentures fit properly. Poor fitting dentures can lead to excess saliva mucking up the corners of your mouth, leading to angular cheilitis.
4. Petroleum Jelly
If the corners of your mouth are cracking due to dehydration or your mouth drying out, using a little bit of petroleum jelly in the corners can help. The jelly locks moisture into those areas, as well as helps heal and prevent the cracking in the corners.
While these medical means can help you clean out the cracked corners of mouth causes, there are several natural remedies that can help you with your angular cheilitis.
Home Remedies for Cracks in Corner of Mouth
For those people who don’t want to take a trip to the pharmacy or want to use a natural remedy for the cracks in the corner of the mouth, there are a few treatments you can make and use in the comfort of your home.
1. Olive Oil
Olive oil has long been used as a home remedy for many things, but you can also use it for the cracked corners of your mouth. A few dabs in the corner of the mouth can help moisten the cracks, and the vitamin content can help repair the cracks.
2. Honey
Another widely used natural remedy, in this case, honey’s anti-bacterial and antiseptic properties, can help clean up bacterial infections. This remedy works best if you apply honey to the cracks and let it sit for around 10 to 15 minutes and then clean the honey off.
3. Aloe Vera
Aloe vera is great for healing damaged skin. Take one aloe vera leaf and refrigerate it for a few hours. Take the leaf out of the fridge and cut the leaf.
Squeeze out some of the aloe vera gel and use a cotton swab to place some of the gel into the cracked areas of the corners of your mouth. Let the gel dry for 15 to 20 minutes. Then, wipe the gel away.
Repeat this method for a few days (twice a day for a week or two should help).
4. Cocoa Butter
Natural cocoa butter can help heal and moisturize angular cheilitis.
5. Cucumber
Cucumber can help moisturize dry skin as well as alleviate some of the discomforts that come with angular cheilitis.
6. Neem Leaves
Leaves of the neem plant can be used to help clean out angular cheilitis-causing infections. Take one neem leaf and crush it until it is relieved of its juice. Apply the juice to the cracks in the corners of the mouth.
Hopefully, these home remedies might be able to help you clean out your problems with angular cheilitis.
Angular Cheilitis Can Hurt But it Doesn’t Have To
Angular cheilitis can be ugly. It can be painful. It can be gross. But luckily, between the medical treatments and the numerous home remedies that are available to you, it doesn’t have to be.
It’s easily treatable and can easily be cleaned up. All you have to do is a little bit of work. Hopefully, we’ve provided you with the tools that you can use to treat your angular cheilitis and get your mouth back to its healthy self.
Also Read:
Sources:
“Cracked Corners of Mouth,” Med-Health; http://www.med-health.net/Cracked-Corners-Of-Mouth.html
“Angular Cheilitis,” WebMD, July 12, 2016; http://www.webmd.com/oral-health/angular-cheilitis#2
“10 Best Home Remedies for Angular Cheilitis,” Home Remedy Shop, November 15, 2013; https://homeremedyshop.com/10-best-home-remedies-for-angular-cheilitis/
“Cracked Corners of Mouth,” Med-Health; http://www.med-health.net/Cracked-Corners-Of-Mouth.html
“Angular Cheilitis,” WebMD, July 12, 2016; http://www.webmd.com/oral-health/angular-cheilitis#2
“10 Best Home Remedies for Angular Cheilitis,” Home Remedy Shop, November 15, 2013; https://homeremedyshop.com/10-best-home-remedies-for-angular-cheilitis/
Created: 21st November 2015 | Last Updated: 6th July 2016
Introduction
Fingertips Cracking Open
While there are many conditions that can cause skin peeling, this chapter, which is set out as below, focuses on the less common, chronic peelings conditions such as the Peeling Skin syndromes. |
Clinical findings
ACRAL PEELING
There are several common conditions associated with acral peeling, eg flare-ups of hand / foot eczema, and juvenile plantar dermatosis. In the acutely unwell child it is important to consider scarlet fever, and, rarely, Kawasaki disease. Other conditions to be aware of include the following:
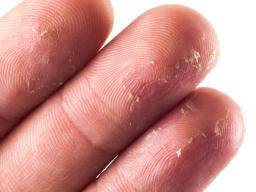
Keratolysis exfoliativa
- This is a common condition, mainly seen in young adults over summer months, and probably more often in those who sweat more
- Lesions present as small white rings or very superficial blisters on the fingers or palms, which soon peel off. The soles are less frequently affected
- The condition is self-limiting, and can be improved with the use of emollients
The Acral Peeling Skin syndrome (APSS)
- Congenital orfamilial acral peeling is extremely rare
- It is an autosomal recessive condition. This means that a person with APSS has inherited a defective copy of the gene from both parents
- The signs and symptoms of peeling skin usually appear soon after birth, but they may also develop later in life
- The main symptom is painless peeling of the skin on the hands and feet. Patients may also experience itching and erythema. Symptoms can be made worse with exposure to water, perspiration, heat, or friction
- One of the main differential diagnoses is localised epidermolysis bullosa simplex
Oudtshoorn disease (syn. keratolytic winter erythema)
- Is a rare autosomal dominant condition that was first described in the Oudtshoorn district of Cape Provence, South Africa
- Symptoms tend to present anywhere from infancy through to early adult life
- Unlike with the Peeling Skin syndromes, the main exacerbations are during cold, dry climatic periods
- The condition is characterised clinically by intermittent and recurrent centrifugal peeling with erythema, particularly of the palms and soles
- In more severe cases, similar patches can be found extending up the limbs to the buttocks and trunk. Lesions can also be annular or polycyclic
GENERALISED PEELING
In addition to the Staphylococcal Scalded Skin syndrome, Stevens Johnson syndrome / toxic epidermal necrolysis, and pustular psoriasis, generalised skin peeling can follow on from a number of widespread inflammatory and bullous eruptions. The following are rare, chronic, scaling conditions:
Peeling Skin syndromes (PSS)
- The Peeling Skin Syndrome (PSS) refers to a group of rare autosomal recessive conditions characterised by episodic or persistent, superficial, asymptomatic, spontaneous peeling of the skin and histologically by a separation of the stratum corneum from the stratum granulosum at the subcorneal level. PSS presents with either an acral (as described earlier) or generalised distribution (or both), and can be non-inflammatory (type A) or inflammatory (type B). Some cases remain difficult to classify
- Symptoms usually present at birth or in early childhood, and then becomes persistent or episodic
- Spontaneous, superficial, painless skin peeling represents the main symptom of this cutaneous disorder
- In the generalised form, the peeling is widespread, with the palms and soles, usually, but not always, spared
- Symptoms tend to be exacerbated in the summer
- There are two main types of the generalised Peeling Skin syndrome:
Type A (non-inflammatory) PSS
- Generalised asymptomatic peeling of the trunk, limbs and occasionally the face
- Histological examination shows an orthokeratotic epidermis with a separation that occurs either within the lower part of the stratum corneum or just above the granular layer
Type B (inflammatory) PSS
- This is characterised by erythematous migratory patches with a peeling border, pruritus, and a tendency towards atopy
- Histology can show an absence of the stratum corneum or a few layers of parakeratosis, which tend to be separated from the stratum granulosum. Psoriasiform acanthosis and perivascular infiltration with mononuclear leucocytes can also be seen
Erythrokeratoderma
- Is the association between localised hyperkeratotic plaques, distinct areas of erythema, and sometimes peeling
- The clinically and genetically heterogeneous group of erythrokeratodermas encompasses several rare genetic skin disorders, including autosomal dominant erythrokeratoderma variabilis and progressive symmetric erythrokeratoderma
- The majority of patients present in infancy
- The skin lesions of erythrokeratoderma variabilis and progressive symmetric erythrokeratoderma show many similarities
Erythrokeratoderma variabilis (EKV)
- Most cases present initially with well-circumscribed, annular or polycyclic erythematous patches. Episodes usually persist for minutes to hours, although may last for days. Fine scaling or peeling may be present. There is a very marked variation in the number, size, shape, distribution and location of the lesions
- Over time the hyperkeratosis develops, which may be generalised or localised with well-defined, yellow-brown, thickened, rough, hyperkeratotic plaques, which have accentuated skin markings. The most commonly affected pattern is a symmetrical involvement of the extensor surfaces, lateral trunk and buttocks. The flexures, face, and scalp are generally spared. The plaques are relatively stable and last for months to years, but they can also clear completely
- In about 50% of cases the hyperkeratosis involves the palms and soles, and this is often associated with peeling
- Lesions are most prevalent during childhood. Improvement and periodic clearing of the skin are not unusual as the patient ages
Progressive symmetric erythrokeratoderma (PSEK)
- The condition causes fixed, orange-red, hyperkeratotic plaques, which gradually extend through childhood. The most commonly affected sites are the cheeks, upper trunk, buttocks and extensor surfaces
- In contrast to EKV, there is no migratory erythema
- The palms and soles are often affected
Ichthyosis
- The ichthyoses are discussed in the related chapter
- They are generally associated with scaling as opposed to peeling, although Netherton's syndrome is characterised by variable degrees of erythema, with episodic skin peeling, and later a characteristic serpiginous migratory annular/polycyclic rash with double-edged scale
Images
Please click on images to enlarge or download. The PCDS would like to thank Dermatoweb, DermQuest (Galderma), and others who have contributed images. All named individuals and organisations maintain copyright for the relevant images. This website is non-profit and holds the images for educational purposes only. Any image downloaded must only be used for teaching purposes and not for commercial use. Notice and credit must be given to the PCDS or other named contributor. Please follow this link if you have any high-quality images that you can contribute to the website.
Figure: 1 Keratolysis exfoliativa |
Figure: 2 Keratolysis exfoliativa |
Figure: 3 Keratolysis exfoliativa |
Figure: 4 Acral Peeling Skin syndrome |
Figure: 5 Acral Peeling Skin syndrome The two images on the right are epidermolysis bullosa simplex |
Figure: 6 Juvenile plantar dermatosis |
Figure: 7 Oudtshoorn disease |
Figure: 8 Peeling Skin syndrome - type A (non-inflammatory) Original source Indian Journal of Dermatology, Venereology and Leprology |
Figure: 9 Peeling Skin syndrome - type A (non-inflammatory) Peeling of superficial skin over the volar aspect of the forearm after induced mild trauma Copied with kind permission from Dr Manish Bansal |
Figure: 10 Peeling skin syndrome - type B (inflammatory) |
Figure: 11 Peeling skin syndrome - type B (inflammatory) Original source Indian Journal of Dermatology, Venereology and Leprology |
Figure: 12 Search results secret for mac. Netherton's syndrome |
Figure: 13 Erythrokeratoderma variabilis |
Figure: 14 Same patient as above - treated with acitretin |
Figure: 15 Progressive symmetric erythrokeratoderma Original source Indian Journal of Dermatology |
Figure: 16 Progressive symmetric erythrokeratoderma Original source Indian Journal of Dermatology |
Figure: 17 Progressive symmetric erythrokeratoderma Peeling present Original source Indian Journal of Dermatology |
Management
Why Are My Fingers Peeling And Cracking
- There is no known treatment that can cure these conditions
- Emollients can provide symptomatic relief
- Treatment sometimes provided in Secondary Care are the retinoids (mainly acitretin) and occasionally phototherapy, which can substantially improve symptoms in some patients
